Telehealth isn’t a pandemic era fad. The global telehealth market is expected to reach around $455 billion in 2030 (up from $123 billion in 2024), and virtual care has become a standard part of healthcare delivery. Post-pandemic, telehealth adoption stabilized at a higher baseline than before – for example, telemedicine still comprised roughly 6% of all medical visits in 2023 (after peaking during COVID). Certain fields like mental health saw especially high uptake, with 38% of psychiatric visits done remotely by 2023. Crucially, supportive regulations and investments in digital health are fueling continued growth. In the U.S., Medicare and insurers expanded coverage for telehealth, and forecasts suggest telehealth could account for 25–30% of all visits by 2026 given the right regulatory support. Globally, governments are also modernizing rules to integrate virtual care into mainstream practice.
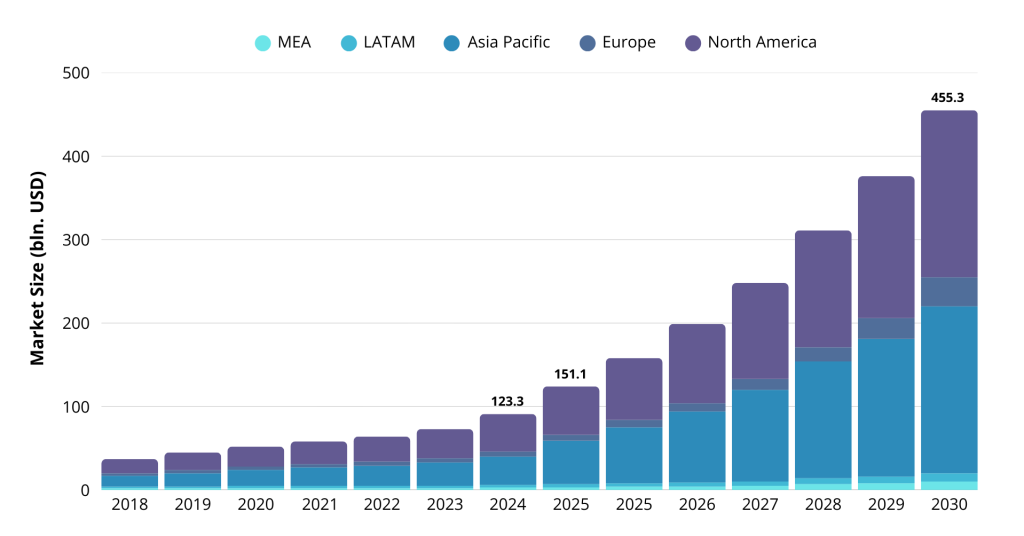
The bottom line – telehealth is here to stay and growing fast, making now a prime time to invest in telehealth app development.
What is a telehealth app?
A telehealth (or telemedicine) app is a digital platform that provides remote healthcare services by connecting patients and providers via technology. Essentially, it allows patients to consult with doctors from home via secure video or chat rather than in person. Modern telemedicine apps offer much more than basic video calls; they often include features such as appointment scheduling, access to electronic health records, digital prescriptions, and remote monitoring of vital signs. In short, a telehealth app serves as a complete virtual clinic, supporting everything from routine check-ups and therapy sessions to chronic disease management and prescription refills. These platforms must also comply with strict privacy regulations such as HIPAA and GDPR, and integrate with healthcare workflows. By 2025, cutting-edge telehealth solutions will leverage AI for diagnostics and the Internet of Things (IoT) for real-time patient data, reflecting an evolution from simple video chat tools to sophisticated healthcare ecosystems.
This guide will teach you how to plan, design and launch a telehealth application. We will cover technical choices, compliance, and user experience considerations to help you create a competitive product. We will also discuss the business benefits and future trends in telehealth and explain how a seasoned partner such as Intersog, a global healthcare software development company, can help you deliver a HIPAA-compliant, scalable telehealth platform. Let’s dive in.
Step 1: Define the Purpose and Use Cases
Building a successful telehealth app starts with a clear purpose and target use cases. Telehealth is a broad field – you need to decide what kind of healthcare services your app will provide and to whom. Will it be a general telemedicine platform for everyday illnesses, a specialized app for mental health counseling, or perhaps a tool for managing chronic conditions? Defining this upfront will guide your feature selection and development priorities.
Common categories include:
- General Consultation Platforms: These connect patients with primary care doctors or urgent care providers for common health issues (think Teladoc or Intersog’s Salus Telehealth). They handle a bit of everything – from sniffles and rashes to follow-up visits – and often operate 24/7 with on-demand video consultations.
- Mental Health & Therapy Apps: Focused on behavioral health services, these enable remote counseling, psychiatry, or addiction therapy via secure video or chat. For example, apps like BetterHelp provide virtual therapy sessions with licensed counselors. Such apps may allow anonymity or self-scheduling with specialists and must ensure extra privacy for sensitive conversations.
- Chronic Disease Management: These telehealth solutions support patients with long-term conditions like diabetes, hypertension, or heart disease. They often integrate remote patient monitoring (RPM) – e.g. Bluetooth glucose meters or blood pressure cuffs – to continuously track vitals. Clinicians can monitor trends and intervene early. Chronic care apps also facilitate regular virtual check-ins, medication reminders, and educational content to improve treatment adherence.
- Telepharmacy & Prescription Delivery: Some telehealth services center on medication management – for instance, apps that let patients consult a doctor and get an e-prescription delivered to their pharmacy or doorstep. Especially since 2020, many countries allow doctors to prescribe medicines via telehealth. An app might combine video consults with pharmacy integrations for seamless e-prescriptions and home delivery.
- Remote Monitoring & Post-Acute Care: Beyond live visits, telehealth extends to continuous remote care. Examples include post-surgery follow-up apps, rehabilitation/physiotherapy apps, or home health platforms where nurses monitor patients after hospital discharge. These rely on devices (wearables, sensors) sending data to the app, where providers can track recovery progress and provide guidance remotely.
- Specialty Telemedicine: Telehealth is also expanding into niches like teledermatology (patients send skin photos for review), teleoncology (virtual tumor board consults), telenursing, tele-dentistry, etc. Each specialty might need custom features (e.g. high-resolution imaging for dermatology). If your project targets a specific specialty, you’ll need to tailor the app’s workflow to those clinical needs.
Identify Your Users and Business Model
Think about who will use your app and how it generates value. Is it directly for consumers/patients, or for hospitals and clinicians?
A direct-to-consumer app (B2C) might need features like patient self-registration, doctor marketplace and ratings, and card payment processing by patients. A clinic-focused app (B2B) might prioritize EHR integration and multi-user support for doctors, nurses, and admins within an organization.
Also decide on the care delivery model – on-demand vs. scheduled visits, one-to-one vs. group sessions, etc., as this affects feature requirements (e.g. on-demand services need a queue and routing system to connect patients to available providers).
Business Model Impact on Features
Your revenue model will influence feature priorities. For example, if you plan a subscription model (patients pay a monthly fee for unlimited telehealth, as seen in some concierge telemedicine services), you’ll need subscription management, usage tracking, and perhaps tiered feature access. If you go for pay-per-visit (transaction-based), you’ll focus on robust payment processing and maybe insurance claims handling. A B2B SaaS model (licensing your platform to clinics) might require white-labeling capabilities and multi-tenant support.
It’s wise to sketch a Business Model Canvas for your telehealth app outlining key segments, value propositions, and revenue streams – this exercise will clarify which features are “must-have” versus “nice-to-have” for your particular solution.
At this stage, take the time to gather input from relevant stakeholders, such as doctors, patients and payers. Understanding the needs of your target users will ensure that your telehealth app is designed to solve real problems. For instance, older people with chronic illnesses may prioritise easy device integration and caregiver access, whereas busy young professionals might prioritise on-demand convenience and quick prescription refills. Clearly defining your use cases and business goals in Step 1 will inform all subsequent development steps.
Step 2: Must-Have Features in 2025
By 2025, a telehealth app needs to provide a comprehensive and user-friendly virtual care experience. Patients and providers now expect telehealth platforms to replicate the functions of an in-person visit and offer the efficiency of digital tools.
Below, we outline the features and functionalities that your telehealth app must include by 2025. We will also present a comparison table to distinguish between core and advanced features.
HD Video and Audio Consultations
High-quality, real-time video calling is the backbone of telehealth. Your app should facilitate secure live video and audio sessions between patients and clinicians. Aim for low-latency HD video that can adapt to varying network speeds (implement adaptive bitrate streaming to ensure stable calls for patients with weaker internet connections).
Common features include one-click join (no complex setup), the ability to invite multiple parties (e.g. a specialist or an interpreter) and screen sharing (so doctors can review charts or images with patients). Consider offering an in-call chat feature for sending links or notes during the consultation.
Also consider offering recording capabilities (with patient consent) for quality assurance purposes or to allow patients to replay their doctor’s instructions. All video sessions must be encrypted and HIPAA-compliant – you could use frameworks such as WebRTC or services such as Twilio, which specialise in secure medical video.
Appointment Scheduling & Reminders
A robust scheduling module is essential for any telehealth platform. Patients should be able to book appointments with their preferred provider or based on availability. The scheduling system must prevent double-booking and synchronise in real time if providers have other calendars.
Include features such as appointment reminders via text message, email or push notifications to reduce the number of patients who do not attend appointments (many telehealth platforms have reduced no-show rates thanks to automated reminders).
Also consider implementing a waiting list system so that if a cancellation occurs, another patient can take that slot.
For multi-clinic platforms, enable clinic administrators to set providers' schedules and allow patients to select time slots.
Users in 2025 will also appreciate convenient features such as calendar integration (e.g. one-tap add to Google/Outlook calendar) and the ability to reschedule or cancel within the app. Smooth scheduling improves both the patient experience and provider utilisation rates.
Electronic Prescriptions (e-Prescribing)
If your telehealth app involves doctors prescribing medication, you should integrate an e-prescription feature. This enables providers to send prescriptions directly to patients' chosen pharmacies via the app. This improves both accuracy and convenience. Depending on the country, your app may need to integrate with e-prescribing networks or pharmacy APIs.
Include features such as medication selection (with dosage and form), checking for drug interactions or allergies (if you have the relevant data) and confirmation when the pharmacy receives the prescription. As many telehealth visits result in a prescription, this would be a significant added value.

Ensure compliance with local e-prescription regulations and include the necessary information. For example, in the US, controlled substances require special handling in accordance with EPCS standards.
By 2025, patients will often expect any needed medication to be seamlessly sent to their pharmacy after an online consultation – telehealth platforms like Teladoc and MDLive have offered this for years. Providing eRx in-app enhances patient satisfaction and closes the care loop.
AI-Powered Symptom Checker & Chatbots
A cutting-edge feature of 2025 is the integration of artificial intelligence (AI) to provide preliminary assistance and triage.
AI symptom checker chatbots can interact with patients 24/7, asking about symptoms and medical history in order to provide initial guidance and advice on urgency. For example, prior to a consultation, an AI bot could gather information such as “What symptoms are you experiencing?”, “How long have you been experiencing these symptoms?” and “Rate your pain”, before suggesting possible causes and whether the patient should see a GP or specialist. The Cleveland Clinic’s virtual triage AI achieved 94% diagnostic accuracy in identifying patient needs, demonstrating how far this technology has advanced. Including an AI symptom checker can improve patient engagement and help prioritise care, as urgent cases can be flagged for immediate attention.
Chatbots can also answer common questions ('How do I prepare for my telehealth visit?') or provide mental health exercises for anxiety, etc., eliminating the need to wait for a human response.
When implementing AI, it is important to ensure that it is thoroughly tested for medical accuracy and bias, and that it is clear that it is not a doctor, but rather a support tool that suggests next steps. When used effectively, AI assistants can save doctors time by pre-collecting information or handling simple follow-ups, and empower patients by providing instant feedback.
Remote Patient Monitoring (RPM)
Telehealth in 2025 often extends beyond the video visit via IoT and medical device connectivity. Must-have telehealth apps integrate with remote monitoring devices to track patients’ health data in real time. For example, a chronic care app might connect to a patient’s Bluetooth blood pressure cuff, blood glucose monitor, pulse oximeter, or wearable fitness tracker.
The app can collect vital readings and display them on a dashboard for doctors and patients. Set up real-time alerts for out-of-range values (e.g. heart rate too high) so that the care team is notified promptly. This continuous monitoring is invaluable for managing chronic conditions and post-operative recovery – it turns telehealth from a series of isolated visits into a continuous care continuum. Your app might use APIs or SDKs from device manufacturers or general standards like Bluetooth Low Energy for wearables. Data from RPM devices should be stored securely and visualized clearly (trends, charts).

By incorporating RPM, your telehealth platform can significantly improve outcomes through proactive care. (Note: Ensure any device you integrate has regulatory approval if needed, and build in patient consent for data sharing.)
Payment & Insurance Integration
If your telehealth service is paid for (as most are), you need secure and convenient in-app payment processing. Core features include accepting credit and debit cards, as well as digital payments, for self-paying patients. Using a trusted gateway, such as Stripe or PayPal, makes this easier.
Many telehealth apps also handle insurance billing. For example, a US patient can enter their insurance details and the platform will verify their coverage or collect a co-payment. In 2025, integration with insurance APIs is expected, or at least the ability to provide patients with an electronic receipt containing the correct codes to file claims.
If you are targeting markets such as the EU or Israel with national insurance systems, you may need to integrate with these systems or provide documentation for reimbursement.
For B2B models, the clinic may pay a subscription so that patients don't have to pay; in this case, your platform should support invoicing the B2B client. Also consider telehealth CPT codes and modifiers for insurance billing, if relevant.
The key is to make payments seamless and secure: patients should feel confident about entering card information (use PCI-compliant processors) and understand what they will be charged (transparent pricing). Likewise, providers should be able to get paid easily for their services through the app’s billing system. Offering options like Apple Pay or Google Pay for one-tap payments can help to reduce barriers to using your telehealth service.
Patient Data Analytics & Dashboards
Data is a big advantage of digital health. Include features for patient data analytics that provide insights to providers and even patients themselves.
For clinicians, an admin dashboard could show metrics like number of consultations, patient outcome trends, or flag high-risk patients (for example, an RPM dashboard highlighting which diabetes patients had consistently high glucose readings this week).
Patients might get their own health dashboard – a summary of their vitals, past visit notes, upcoming appointments, and perhaps health tips or goal tracking.
Incorporating analytics can improve care: e.g. using predictive analytics to identify patients who might need intervention. In 2025, machine learning can crunch telehealth data to predict things like which patients are at risk of hospitalization. Even simpler, giving doctors charts of a patient’s readings over time helps in decision-making.
Ensure that dashboards are intuitive and focus on actionable information. You might implement role-based dashboards (one view for a doctor with multiple patients vs. a personal view for a single patient).
Multilingual & Accessibility Features
Telehealth apps must cater for diverse populations. Supporting different languages and ensuring accessibility is no longer optional – it’s essential to serve all patients.
Multilingual capability enables your UI to display in multiple languages and offer real-time translation during consultations. Communities with limited English proficiency have previously encountered obstacles in telemedicine, but technology such as AI translation services can now enable doctors and patients to communicate in their native languages with live captioning or interpreter integration. At a minimum, consider offering your app in the main languages used by your users (Spanish, French, etc.) and ensure that providers can upload notes in these languages.
Accessibility is equally critical: design your UX to be usable by people with disabilities. This includes supporting screen readers for blind users, offering adjustable font sizes and high-contrast modes for visually impaired users, and ensuring that interactive elements can be operated via voice or keyboard input for users who cannot use a touchscreen.
Compliance with WCAG 2.1 AA standards is a good benchmark [39]. Features such as closed captions on video calls, visual cues in addition to audio alerts and simple navigation benefit not just disabled users, but everyone.
Also consider the elderly: use larger default text and straightforward language, avoiding medical jargon where possible, and provide clear guidance at each step, perhaps even offering a tutorial mode. By building in multilingual and accessibility features from the outset, telehealth can reach a wider audience and fulfil an important ethical and regulatory mandate.
HIPAA/GDPR-Compliant Security
Last but certainly not least, top-notch security and privacy is a must-have feature set woven throughout your app. Healthcare data is highly sensitive, and users need to trust that their information is protected. Your app must adhere to HIPAA (in the U.S.) and GDPR (in Europe), as well as any other local privacy laws, from day one.
Core security features include end-to-end encryption for all communication (video, chat, file transfers) so that eavesdroppers can’t read data.
Secure user authentication is needed – implement multi-factor authentication (e.g. SMS or authenticator code) for providers and perhaps patients, and consider biometric login support (fingerprint/FaceID) for mobile apps.
Use role-based access controls so that, for example, only authorized staff can view certain patient records.
The app should maintain audit logs of access to patient data (this is required by HIPAA) – log who accessed what and when.
Other features include automatic logoff after inactivity, secure password policies, and data wipe/lockout features if a device is lost.
On the backend, encrypt data at rest in your databases (using strong encryption like AES-256) and in transit (TLS 1.2/1.3 for all API calls).
Provide clear privacy consent forms within the app for patients to agree to telehealth and data usage policies (GDPR requires explicit consent for data processing).
Essentially, bake security and compliance into every feature – for instance, if you have video calling, ensure the video service provider will sign a Business Associate Agreement (BAA) for HIPAA. If you have cloud storage, use HIPAA-compliant cloud services (AWS, Azure, GCP offer healthcare compliance programs). By treating security as a core feature, you protect your users and avoid legal pitfalls. Patients will share health details only if they feel their privacy is respected, so make your app’s security a selling point.
To summarize the feature set, here is a table comparing core vs. advanced features for a telehealth app in 2025:
| Core Features (Baseline) | Advanced Features (2025) |
| HD Video & Audio Calls – Secure, real-time virtual consultations with high-quality video | AI Symptom Checker & Chatbot – Intelligent triage assistant to assess patient symptoms and answer FAQs |
| Scheduling & Reminders – Patient self-scheduling, calendar sync, and automated appointment reminders | Predictive Analytics Dashboards – Data-driven insights and risk prediction for patient populations |
| Secure Messaging & Chat – Encrypted text/chat between patient and provider for follow-ups and sharing info | Remote Monitoring Integration (IoT) – Connectivity to wearables and medical devices for continuous patient data streaming |
| Electronic Prescriptions (eRx) – Digital prescription transmission to pharmacies, improving convenience and accuracy | EHR Integration (FHIR/HL7) – Seamless data exchange with electronic health record systems and health information networks |
| Payment Processing – In-app payments (credit card, etc.) and/or insurance co-pay handling in a PCI-compliant manner | Insurance Claims & Eligibility – Advanced integration to verify insurance coverage and submit claims for telehealth visits |
| Basic Health Records – Patient profile with medical history, and ability for provider to record notes/prescriptions | Multilingual & Real-Time Translation – Support for multiple languages and AI-driven translation during consultations |
| HIPAA-Compliant Security – End-to-end encryption, user authentication, audit logs, and data protection measures | Enhanced Accessibility Features – Voice command interface, screen reader optimization, and other assistive tech for inclusive design |
Remember that what is considered "advanced" today may become standard tomorrow. AI chatbots and wearable integration, for example, are quickly becoming standard as telehealth providers compete based on innovation. When planning your minimum viable product (MVP), include all the core features so that your app delivers the fundamental telehealth experience. Then, consider which advanced features align with your vision and budget; you may roll those out in phases. In any case, the above features form a blueprint for a complete telehealth solution in 2025.
Step 3: Choose Technology Stack
With your feature requirements in mind, the next step is to select the technology stack with which to build your telehealth app. Your choices regarding the front end, back end, cloud, and integrations will affect your app’s performance, scalability, and ease of development. In the healthcare industry, it is also important to consider technologies that support high security and compliance. Below, we break down the tech stack considerations.
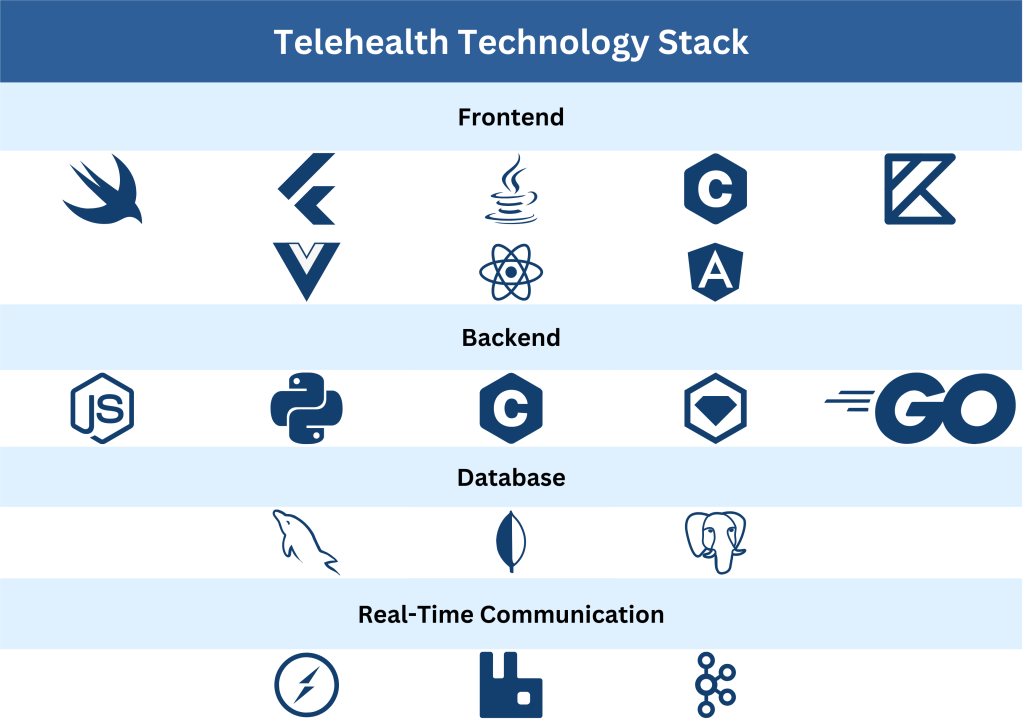
Frontend (Client-side)
This is what end users (patients, providers, admins) interact with – the mobile app or web interface. For mobile apps, you have to decide between native development or cross-platform:
- Native Mobile: Developing separately for iOS (Swift/Objective-C) and Android (Kotlin/Java) can yield the best performance and fully leverage device capabilities (camera, Bluetooth for devices, etc.). Native is often chosen if you need very fine-tuned experiences or must integrate deeply with OS features.
- Cross-Platform Mobile: Frameworks like React Native and Flutter allow you to build one codebase for both iOS and Android. In telehealth, where time-to-market is crucial, cross-platform is popular. React Native is widely used in healthcare apps for its performance and large ecosystem. Flutter offers a rich UI toolkit and can achieve near-native speed as well. These save development effort, though for extremely complex apps you might sprinkle in some native modules.
- Web Application: In addition to mobile, many telehealth solutions have a web app (for accessing via browser on a laptop/desktop). Front-end web technologies include React.js, Angular, or Vue.js. React.js is a common choice for building dynamic health dashboards and video call interfaces on the web. Modern web frameworks can create responsive apps that work across screen sizes, which is great for provider portals or patient access without installing an app.
- UI Frameworks: Consider using component libraries or design systems (e.g. Material-UI for React, Google’s Flutter widgets, etc.) to speed up development of common elements like forms, buttons, modals, etc. Also ensure whichever front-end tech you choose supports accessibility features and internationalization (most do).
In summary, choose a front-end stack that aligns with your team’s expertise and target platforms. Many telehealth startups opt for React Native + React web for consistency, or Flutter for a unified UI. If you foresee heavy use of platform-specific features (like an Apple Watch app down the line, or advanced camera AR on iOS), factor that in. The goal is a smooth, responsive UI that can handle video streams, real-time updates (for chats or device readings), and complex forms – so pick technologies known for performance and community support.
Backend (Server-side)
The backend is the engine behind your app - it handles business logic, database operations, integrations with third-party APIs, and so on. Key backend choices include:
- Programming Language & Framework: Common choices in 2025 for telehealth include Node.js (JavaScript/TypeScript), Python (Django or Flask), Java (Spring Boot), or C# .NET Core, among others. Each has its merits:
- Node.js is great for real-time applications and can use frameworks like Express or NestJS. It’s event-driven and handles WebSockets (for chat or live updates) well. Many startups like Node for its speed in prototyping and using one language (JS) across front and back.
- Python with Django is a strong option for healthcare because of Django’s robust security features and rapid development pace. Python also has many libraries for healthcare and AI, which might be useful if you integrate machine learning (e.g. symptom checker logic). Django can enforce secure practices by default and is well-suited for building RESTful APIs quickly.
- Java (Spring Boot) or C# .NET are enterprise-grade choices. If you anticipate needing enterprise integration or if your team is experienced in these, they offer scalability and a strong type-safe environment. Large hospital systems often use Java or .NET for their reliability and tooling.
- Other stacks: You might also encounter Ruby on Rails (good for rapid development, though less common in new health projects today) or Go (for microservices needing high performance).
- The key is to pick a backend stack that can handle high concurrency (imagine dozens of video calls and device data streaming simultaneously), is known for security, and matches your developers’ skills. For example, Python/Django is recommended for healthcare apps due to robust security libraries and ease of meeting compliance.
- Database: Healthcare apps deal with various data types – structured records, unstructured chat logs, perhaps images (x-rays, etc.). Often a combination of databases is used:
- A relational database like PostgreSQL or MySQL for core patient and visit data. PostgreSQL is popular for its reliability and support for JSON fields (to store semi-structured data). It enforces schema, which is good for structured medical info (patients, appointments, prescriptions).
- A NoSQL database like MongoDB can be useful for storing things like chat transcripts, wearable data streams, or other flexible schemas. Mongo’s document model can adapt to varying data from different devices, for example.
- You may also consider in-memory databases or caches like Redis for fast access to certain data (session tokens, real-time metrics). Redis can also assist in managing real-time signaling for video or chat (e.g. a pub/sub pattern).
- If dealing with large files (imaging or lengthy recordings), a storage service (like AWS S3 or Azure Blob) might be part of your stack.
- Ensure your database selection can support encryption at rest and robust backup/restore. Many cloud providers offer managed database services that are compliant (like AWS RDS with encryption and backups).
- Real-Time Communication: Telehealth apps rely on real-time events (incoming call requests, chat messages, device data updates). For this, your backend might use WebSocket technology or specialized messaging systems:
- Socket.io (on Node.js) or similar WebSocket frameworks can maintain live connections for instant notifications.
- Sometimes a separate message broker (like RabbitMQ or Kafka) is used to manage event streams, especially if you have microservices.
- Use of WebRTC for video is largely on the client side, but a signaling server (maybe using Node or even a service from a provider) will coordinate the peer connections.
- Microservices vs Monolith: A smaller telehealth MVP might start as a monolithic app (all backend functions in one codebase). As you scale, you could split services (e.g., a service for video handling, another for data analytics, etc.). Technologies like Docker and Kubernetes become relevant if containerizing microservices for scalability. However, early on, simplicity is fine – ensure your architecture can scale later when needed.
In summary, choose backend technologies that are scalable, secure, and integration-friendly. Cloud platforms often support all the above languages – e.g. AWS, Azure, GCP – and provide compliance certifications. Many telehealth developers favor high-level frameworks (Django, Node/Express) to get a lot done with less code, but ensure your team can implement strict security controls regardless of stack.
Cloud Hosting and Infrastructure
Hosting a telehealth app requires reliable infrastructure, ideally with cloud scalability and compliance support. Cloud platforms like Amazon Web Services (AWS), Microsoft Azure, or Google Cloud Platform (GCP) are commonly used. They offer server hosting, databases, storage, and built-in compliance options:
- AWS has specific HIPAA-eligible services (and will sign a Business Associate Agreement) – commonly used ones include EC2 or ECS for compute, RDS for databases, S3 for storage, etc. AWS also offers Chime SDK for video calls if you prefer that to third-party.
- Azure likewise has a full HIPAA compliance portfolio and is popular with enterprise healthcare (integrates well with Microsoft’s healthcare tools).
- GCP has a strong data and AI suite, which could be useful if integrating analytics or ML, and they also support HIPAA compliance.
Choosing a cloud means you don’t have to manage physical servers and you can scale on demand (e.g. spin up more instances during peak usage like daytime hours). It also simplifies deploying updates via CI/CD pipelines.
DevOps and CI/CD
Implement a CI/CD pipeline so that you can frequently deploy updates and security patches. Tools like GitHub Actions, Jenkins, or GitLab CI can automate testing and deployment. Containerization (Docker) and orchestration (Kubernetes) are often used to manage deployments at scale – for instance, if you containerize your app, Kubernetes can ensure high availability and scale pods based on load.
- Monitoring & Logging: Cloud platforms have monitoring tools (like AWS CloudWatch, Azure Monitor) to track uptime, performance, and get alerts on issues. Implementing an ELK stack (Elasticsearch, Logstash, Kibana) is a good practice for analyzing logs and audit trails. This ties into compliance – you need to log access to data, and these logs should be stored securely (and reviewed).
- Infrastructure as Code: Consider using Terraform or CloudFormation to manage your infrastructure as code for consistency and easier modifications as you grow.
In short, leveraging cloud infrastructure will help you meet the reliability and security requirements of telehealth without reinventing the wheel. Ensure that whichever provider you use, you enable encryption, backups, and regional settings that align with data residency laws (for example, store EU patient data in EU data centers for GDPR compliance).
APIs and Third-Party Integrations
No telehealth app is an island – you will likely integrate several external services via APIs to implement certain features quickly:
- Video/Voice APIs: If you don’t build the video calling from scratch with WebRTC, you can use APIs like Twilio, Agora, Vonage (TokBox), or Dolby.io. These provide SDKs to embed live video and are HIPAA-compliant (Twilio and Vonage will sign BAAs, for instance). Using such APIs can drastically shorten development time for the complex video feature – e.g. OpenTok (Vonage) or Agora.io handle multi-party streaming and network traversal for you. Evaluate cost vs. building yourself; many startups start with an API and later optimize or switch if needed.
- Payment APIs: Stripe and PayPal are popular for handling payments securely. Stripe in particular offers a robust API and has support for one-time or subscription billing. It can also help with storing payment info tokenized (so you’re not handling raw card data). These are PCI-compliant and trusted by users. If you need to handle insurance co-pays or more medical-specific billing, there are platforms like Redox or Eligible API that handle insurance eligibility checks.
- EHR Integrations: Connecting with Electronic Health Records can be critical if your platform is used by existing healthcare facilities. Modern EHR systems (Epic, Cerner, etc.) often support FHIR API endpoints – Fast Healthcare Interoperability Resources is the emerging standard for exchanging health data. Your app could use FHIR APIs to pull a patient’s medical history or push telehealth consultation notes back into the hospital’s EHR. There are integration engines (like Redox or Mulesoft) that can facilitate connecting to various EHRs via HL7, FHIR, or other protocols. If targeting the U.S., understanding SMART on FHIR (for apps inside EHRs) might be useful, but for an independent app, sticking to FHIR REST APIs is usually enough. HL7 FHIR is definitely the way forward for interoperability – plan to support it so your app can talk to any FHIR-compliant system.
- Notifications & Communication: Use services for sending SMS/email notifications. For example, Twilio (for SMS), SendGrid or Mailgun (for emails) to send appointment reminders or verification codes. These need to be configured to meet privacy rules (e.g., not including PHI in plain text messages).
- Maps/Location APIs: If your app involves finding nearby services (like a local pharmacy or lab for tests), integrating with Google Maps API could be useful.
- Analytics & Crash Reporting: Utilize tools like Google Analytics (or better, a HIPAA-compliant analytics solution that doesn’t log personal data) to track usage, and services like Sentry for error/crash reporting to fix issues proactively.
- When choosing third-party APIs, always verify their compliance stance (will they sign a BAA? How do they handle data?). Many healthcare software development companies maintain a vetted list of “safe” libraries and services. The right integrations can save you months of development, so leverage them wisely.
Overall, your technology stack should support the features and scale you need while maintaining high security. Many successful telehealth applications use a stack that includes: A React Native front end, a Node.js or Python back end, a PostgreSQL database, an AWS cloud, Twilio or Agora for video, Stripe for payments, and HL7 FHIR for EHR integration. There is, of course, flexibility — the key is ensuring that all the pieces work together and can meet healthcare compliance requirements. It is often beneficial to consult with experienced architects or a healthcare software development company at this stage because they can recommend reliable technologies and architectures for telehealth platforms. With the right stack in place, you're ready to build a robust telehealth solution.
Step 4: Ensure Compliance & Security

Healthcare is a heavily regulated industry for good reason: we deal with sensitive personal health information (PHI). Any telehealth app must prioritize compliance and security from the ground up. Failing to do so can result in legal penalties, data breaches, and loss of user trust. In this step, we’ll outline the key regulations, such as HIPAA and GDPR, and the security measures you need to implement to keep your platform safe and compliant in different regions, including the USA, the EU, Israel, and beyond.
HIPAA Compliance (USA)
If your app will handle PHI from U.S. patients, it must comply with the Health Insurance Portability and Accountability Act (HIPAA). HIPAA sets strict rules on who can access health data and how it must be protected. Key points:
- Only “covered entities” and their “business associates” can handle PHI – if you’re providing the software to healthcare providers, you likely count as a business associate and will need to sign BAAs with your clients and vendors.
- Implement the Administrative, Physical, and Technical safeguards as outlined by HIPAA. Technical safeguards include measures like access controls (unique user IDs, emergency access procedures), audit controls (logging system activity), integrity controls (protect data from improper alteration), and transmission security (encryption for data in transit). We already discussed many of these in the features and tech stack sections.
- Use HIPAA-compliant infrastructure: host on servers that provide required security and sign a BAA (e.g. AWS, Azure have this). Use encrypted databases and secure backup solutions.
- Ensure any third-party service that touches PHI signs a BAA. For example, if you use Twilio for SMS containing PHI or video, Twilio should be under a BAA to be safe.
- Educate your team on HIPAA as well – often breaches happen due to human error. Have policies for how developers and support staff handle any real patient data.
- Non-compliance is serious: penalties can reach up to $1.5 million per violation and lead to lawsuits. So design your app with a “HIPAA-first” mindset.
- A quick example: Skype or standard Zoom are not HIPAA-compliant by default (no BAA, no guaranteed encryption standard for medical use), which is why healthcare providers need purpose-built telehealth solutions. Your app should fill that gap by being secure from end to end.
GDPR (EU) and European Regulations
If you have users in the European Union, the General Data Protection Regulation (GDPR) comes into play. GDPR is all about data privacy and user control. Some compliance steps for GDPR:
- Obtain explicit consent from users for collecting and processing their personal data (e.g. show clear terms and a consent checkbox when signing up, especially before any sensitive data is collected).
- Allow users to exercise their rights – the right to access their data, rectify errors, and even delete their data (“right to be forgotten”). Your app should have processes to fulfill these requests.
- Minimize data collection: collect only what is necessary for providing the service. For instance, if video visits don’t need storing the video, don’t record it by default. If you do record, have a clear retention policy.
- Ensure data transfers out of the EU (if any) are legal – either host EU user data on EU servers or use approved transfer mechanisms (Standard Contractual Clauses, etc.). Many telehealth providers simply ensure EU data stays in EU data centers to simplify this.
- Appoint a Data Protection Officer (if applicable) and have breach notification processes in place (GDPR requires reporting breaches within 72 hours).
- Other regional laws: Different European countries may have additional e-health regulations, but GDPR is the baseline. Also, keep an eye on the emerging EU AI Act if using AI in healthcare, and the European Health Data Space initiatives that encourage data interoperability (your app supporting FHIR will help align with these future frameworks).
- In short, GDPR compliance means privacy by design – anonymity where possible, security, and giving control to the user over their data.
Local Regulations in Israel and Other Countries
Each country can have its own telehealth guidelines. For example, Israel has been proactive in digital health:
- The Israeli Ministry of Health (MoH) issued a directive (Circular 6/2019) titled “Standards for Operating Remote Health Services (Telehealth-Telemedicine)”. This guideline sets standards to ensure telehealth services are high-quality, accessible, and safe. It covers aspects like: the responsibility of healthcare organizations offering telehealth, required training for telehealth providers, and states that the provider’s responsibility in a remote consult is equivalent to an in-person visit. In practical terms, if you deploy in Israel, you must ensure your app meets those standards (e.g. maintaining patient records of teleconsultations just as you would for clinic visits, verifying the licensing of telehealth providers, etc.).
- Israel’s laws also emphasize data protection – Israel’s Privacy Protection Authority has guidelines on telehealth privacy. Additionally, Israel has its own patient data confidentiality laws that your app must comply with (similar spirit to HIPAA).
- Other examples globally: Canada has PIPEDA, which is similar to GDPR for personal data; in the Middle East, countries like the UAE have health data laws requiring data localization; in Asia, countries like Singapore and Australia have telehealth guidelines and privacy acts. When launching in any new region, research local e-health regulations. Often it boils down to patient consent, data security, and ensuring providers using the platform are licensed appropriately in the patient’s jurisdiction.
- If your app will connect across state or country lines, be mindful of licensing requirements: e.g., U.S. doctors must usually be licensed in the state where the patient is located during the consult. Technology can handle this by matching patient location and provider credentials, or providing warnings. The regulatory landscape is evolving (many places relaxed cross-state telehealth rules during COVID, some are permanent, some not), so keep updated.
Security Best Practices
Compliance sets the minimum required; beyond that, follow industry best practices for cybersecurity. Some key measures to implement:
- End-to-End Encryption: As mentioned, encrypt data everywhere. Use TLS 1.3 for all data in transit (API calls, websockets). For stored data, use strong encryption (AES-256). If using mobile, consider using OS-level encryption for local data storage (and advise users to use device encryption).
- Multi-Factor Authentication (MFA): Especially for providers and admins, enforce MFA on login. Even for patients, offering MFA as an option (via SMS or authenticator apps) can prevent unauthorized account access.
- Secure Session Management: Use short-lived JWT tokens or similar for sessions, secure cookies (HttpOnly, Secure flags), and automatically log users out after a period of inactivity or if credentials change. Prevent multiple concurrent sessions if appropriate and use device recognition for added security.
- Input Validation & Safe Coding: Guard against common vulnerabilities like SQL injection, XSS, CSRF, etc. Use frameworks’ security features and perform code reviews. Given that telehealth apps handle file uploads (images, documents), ensure you virus-scan uploads and restrict file types to avoid malware.
- Regular Security Audits: Conduct penetration testing and vulnerability scanning regularly (at least annually, if not per major update). Hire third-party security experts to audit your application for weaknesses. Compliance might require this (HIPAA doesn’t explicitly, but it’s implied in risk management; other standards like ISO 27001 or SOC2 which some health companies pursue will require audits).
- Incident Response Plan: Have a clear plan for how to respond to a security incident or breach. This includes how to notify users and authorities (HIPAA and GDPR have breach notification rules) and how to patch the issue.
- Data Retention & Disposal: Set policies for how long you retain medical records, recordings, chat logs, etc., in compliance with laws (some data might need to be kept X years; others you may choose to purge sooner to reduce liability). When users request deletion (and it’s allowable by law to delete), actually purge their data from all systems and backups if possible.
- Audit Trails: Maintain logs of system access and data access. For example, log whenever a doctor opens a patient’s record or whenever an admin changes permissions]. These logs should be tamper-evident (write to append-only storage or external monitoring system) so they can be used for forensic analysis if needed.
- Testing for Scale & Performance: A security angle often overlooked – ensure your system can handle high load without failing (since a crash could be a risk for patient safety if people can’t access care). Also protect against DDoS attacks, which can be devastating if your service is taken offline at a critical moment. Cloud providers offer DDoS protection services – use them.
- Role-Based Access Control (RBAC): Build fine-grained access control. For example, within the app, a doctor should only see their own patients (unless a supervisor role needs broader access). A receptionist account might only schedule but not see clinical data. Implement the principle of least privilege throughout.
- Secure Development Lifecycle: Make security a part of development. Train developers on secure coding, use static code analysis tools to catch issues early, and keep dependencies updated (vulnerable third-party libraries are a common leak point – use tools like Dependabot or Snyk to monitor for any known vulnerabilities in your stack).
Remember, trust is paramount in healthcare. Patients need to trust that their sensitive health information is secure on your platform. Providers and clinics need to trust that using your app won't expose them to legal risk. Advertise your compliance and security measures. For example, highlight that your app is HIPAA-compliant, uses encryption, and has passed security audits. This can be a selling point. As you grow, it’s wise to consider certifications. You might pursue HITRUST or ISO 27001 certification to formally demonstrate security, though it's not mandatory. However, it can attract enterprise clients.
In summary, step 4 is an ongoing commitment, not a one-time task. Stay updated on evolving regulations - telehealth rules are still changing post-pandemic - and update your security protocols accordingly. Building a culture of compliance and security creates a strong foundation for your telehealth app’s success and credibility.
Step 5: Design for UX/UI in Healthcare
The design of your telehealth app can make or break it. In healthcare, where your users may include non-tech-savvy patients, busy doctors, and people with disabilities or impairments, a thoughtful user experience (UX) and user interface (UI) is especially critical. The goal is to create an app that is easy to use, comforting, and accessible to all users while meeting the unique needs of healthcare interactions. Below are key principles and tips for designing a great telehealth UX/UI:
- Simplicity and Clarity:
- Medical interactions can be stressful for patients, so your app should not add confusion. Embrace a clean, uncluttered interface with clear labels and instructions.
- Use plain language – for instance, say "Find a Doctor" instead of "Initiate Consultation" if aiming at patients.
- Keep the number of steps low: e.g., booking an appointment should be a quick process with minimal form fields.
- A good practice is to map out user journeys (for a patient and for a provider) and remove any unnecessary friction. For example, if a user must fill a long medical history, consider breaking it into bite-sized steps or optional sections.
- Short paragraphs and big buttons are your friends for readability on mobile. Remember that a significant portion of your audience may be older adults – design for their needs by avoiding small text (aim for a base font size that’s comfortable, maybe 16px+ on mobile) and ensuring good contrast between text and background.
- Patient-Friendly Interfaces:
- Think of your app from the perspective of a patient who may not be feeling well. Reassurance and guidance in UI can improve their experience. For instance, during the onboarding or first use, provide a brief tutorial or tooltips (like “Here’s how to join your video appointment”).
- During a video call, the patient might wonder “Is my camera on? Can the doctor hear me?” – use clear icons (with labels like "Microphone On/Off") and maybe a status that says “You’re in the waiting room – the doctor will join soon” to reduce anxiety.
- Doctor profiles should be easy to browse, with friendly photos and bios, helping patients choose and trust their provider.
- Use empathetic design: perhaps a calming color scheme (many health apps use blues/greens) and imagery that makes users feel at ease (e.g., an icon of a friendly doctor avatar).
- Also, provide feedback for actions – if a patient presses “Book appointment”, show a confirmation like “Appointment booked! Dr. Smith will see you on Tue 10am” and maybe an email/text follow-up. These little details in UX copy and flow make the experience more human.
- Optimized Workflow for Providers:
- On the clinician side, time is of the essence. Design the UI to fit into a medical workflow. For example, a doctor’s screen during a telehealth call might need the patient’s info and chart easily accessible alongside the video feed.
- Consider a split-screen or picture-in-picture mode where the provider can see the patient’s face and also scroll through their recent lab results or enter notes.
- Ensure that entering consultation notes or e-prescribing during/after a call is straightforward (template notes or dropdowns can help with common assessments to save typing).
- Provide shortcuts: e.g., one-click to send a prescription or one-click to schedule a follow-up for that patient.
- If the provider interface will be used by many specialties, gather feedback from a few clinicians to see what information they most need at their fingertips.
- Reduce cognitive load – doctors shouldn’t have to click through many menus; common tasks should be front and center. Arkenea, a telehealth developer, notes that they create separate optimized interfaces for different user roles (patient, provider, admin) so each sees a UI tailored to their needs. Adopting that approach can ensure you’re not giving a one-size-fits-all that fits none.
- Accessibility and Inclusive Design
- We touched on this in features, but from a design perspective, follow accessibility guidelines (WCAG 2.1) diligently.
- Use sufficient color contrast for text (check contrast ratios for compliance).Provide text alternatives for any icons or images (so screen readers can describe them).Support keyboard navigation (some patients might use only a keyboard or assistive switches).For hearing-impaired users, ensure all audio (like doctor’s spoken instructions) could be supplemented with text – maybe allow real-time captioning or a chat summary.For visually impaired, ensure compatibility with screen readers (proper semantic HTML in web, content descriptions in mobile).Testing your app with accessibility tools or even with users who have disabilities is invaluable. Accessibility is not just ethical but often legally required for healthcare apps (ADA compliance in the U.S., for example).Also consider cognitive accessibility – make the interface predictable and consistent. Use common icons (a calendar icon for scheduling, a phone or video icon for calls) so users don’t have to relearn meanings.
Internationalization: design layouts that can handle longer text if translated to another language (German text, for instance, tends to be longer than English). And ensure your design still looks good if the user chooses a larger system font or zoom level.
Features to Enhance UX
Consider some extra design features that can significantly improve user experience in healthcare context:
- Wait-time Indicators: If a patient is in a virtual waiting room, show an indicator like “Dr. Jones will join in approx. 5 minutes” or a simple spinner with a reassuring message. Uncertainty is frustrating, so if the doctor is running late, you might even show a notice or offer the patient an option to reschedule.
- Contextual Help: Little “i” info icons or a help chatbot can assist users if they get stuck. For instance, an info tooltip next to "Enter your symptoms" might say "Describe your issue in a few sentences – e.g., 'I have had a fever for 2 days'." This helps users provide relevant info.
- Dark Mode: Many users appreciate dark mode (light text on dark background), especially if they use the app at night or if providers are on-call in dark environments. Implementing a dark theme toggle can improve comfort. Just ensure colors still meet contrast requirements.
- Feedback Mechanisms: After visits, you might let patients rate the call quality or provide feedback on the consultation. If you include this, design it to be simple (like a 5-star rating or thumbs up/down plus an optional comment). This not only gives you UX insights but also engages the patient.
- Localization of Illustrations: If you use any illustrations or images, consider cultural appropriateness. Healthcare can be sensitive – images of people should be diverse and non-stigmatizing. Also, some cultures interpret colors differently (though blue/green for health is generally safe).
Designing a telehealth app requires balancing functionality with empathy. It's important to meet clinical needs while keeping things intuitive for laypeople. Investing in good UX/UI design and iterating based on user feedback will create a platform that users find easy and enjoyable to use. Happy users are more likely to adopt and stick with the app, which is crucial for the success of a telehealth solution. One final tip: involve real end users (patients and providers) in your design process through interviews or beta tests. Their insights will help you make design decisions that will truly make virtual care more accessible and effective for everyone.
Step 6: Testing and Quality Assurance
Thorough testing and quality assurance (QA) is absolutely critical in healthcare software. A telehealth app is not just another e-commerce site or social app – if something goes wrong, it can directly impact people’s health and safety. You need to be confident that your app works as intended under all reasonable conditions and meets all requirements (functional and regulatory) before it goes live, and continuously thereafter. In this step, we’ll cover the types of testing you should perform and special QA considerations for telehealth.
- Functional Testing (covering all user scenarios):
Ensure every feature works correctly according to specifications. This means testing each user role (patient, doctor, admin, etc.) and all use cases:
For example, create test scenarios for scheduling: patient books, provider sees it, reschedule, cancel, no-show flows. Test video calls: can both parties connect, what if one disconnects, does reconnection work? Test e-prescriptions: does the pharmacy receive it correctly? Essentially, validate all application features across different user roles and scenarios.
Don’t forget edge cases: what if a patient tries to book two appointments at the same time? What if a doctor account is deactivated, can they still log in? Try to break the application in testing so that users won’t in production.
- Exploratory testing by a QA who was not the main developer is useful – they might find issues by using the app in ways developers didn’t anticipate.
- Usability Testing (with real users if possible):
This goes beyond just “does it work” to “is it user-friendly and does it meet user needs.” Ideally, have some doctors and patients do trial runs of the app and gather feedback. Watch how a non-tech-savvy user navigates – do they get stuck anywhere? Do providers feel the workflow is convenient? You may discover, for instance, that patients had trouble finding the “Join Call” button due to wording or placement – you can then tweak the UI.
Usability testing can be done with prototypes earlier, but doing it again on a near-final product is important. Even small improvements (like adding an on-screen message “Your camera is off – tap to turn it on” if the app detects no video) can make a big difference in actual use.
In healthcare, consider a beta pilot: recruit a small clinic or group of users to use the app in real consultations for a couple of weeks, under supervision. Gather their issues and fix them before a wider release.
Also ensure accessibility is tested: have someone use the app with a screen reader, or only keyboard, etc., to verify those features really work in practice. - Performance and Load Testing:
Telehealth apps can be resource-intensive (video streaming) and may face high loads (imagine spikes during a flu season when many patients hop on). Conduct performance tests to ensure the system can handle expected user volumes with acceptable speed.
Use tools to simulate concurrent usage: e.g., simulate 100 video calls happening at once, or 1000 users hitting the login or scheduling system simultaneously. Measure response times and resource usage. This will show if you need to scale infrastructure or optimize code queries.
Test under various network conditions for video calls: simulate low bandwidth or high latency on the client side to see if video quality gracefully degrades (there are network simulation tools or simply test on a throttled connection).
Also test how the system behaves during longer sessions – e.g. a video call lasting 1 hour – to ensure there are no memory leaks or dropped connections over time.
The aim is to ensure reliable operation during peak usage. Telehealth usage can have peaks (e.g., Monday mornings, or during a health scare event) – you want the app to stay responsive and not crash when it’s needed most.
- Security Testing:
As detailed in Step 4, you should engage in penetration testing and vulnerability scanning as part of QA. Security specialists will attempt to find ways to breach your system: SQL injections, XSS attacks, breaking authentication, etc. Also test scenarios like:- Ensure a patient cannot access another patient’s data by modifying an ID in the URL or API call.
- Ensure that even if someone intercepts data, it’s encrypted (e.g., sniff network traffic to confirm video stream is encrypted and that API responses don’t leak more info than they should).
- Test that your server is configured correctly (no open ports that shouldn’t be, proper TLS certificates, no using deprecated protocols).Simulate a lost device: if a phone with the app is stolen, can someone access PHI? (This relates to whether you require login each time or have remote wipe capabilities for critical data).
- Make sure all third-party components are up to date to address known vulnerabilities.
- Any issues found should be fixed and re-tested. Security testing isn’t one-and-done – integrate it into your pipeline (like run automated scans regularly, and do a full pen-test at least annually or before major releases).
- Compliance Testing (Audit and Regulatory QA):
It’s worthwhile to do a compliance audit simulation. For HIPAA, that might mean checking that audit logs are recording everything properly, verifying that all data fields that need encryption are encrypted, and confirming that you can produce reports of access if needed]. For example, ensure that when a patient downloads their data (if you offer that), only their data comes and it’s in a correct format (for interoperability, maybe CCD or FHIR format if applicable).
If you plan to get certifications (like ONC Health IT certification or others), do specific testing against those criteria.
Test your backup and recovery – compliance includes being able to restore data in case of failure. Try a disaster scenario: what if a server goes down? Does the failover work? If not, better to find out in testing than in reality.
If operating across regions, test that the appropriate regional settings are in effect (for instance, a European user’s data stays in the EU database shard, etc., if that’s how you designed it).
This type of testing ensures you are not just functionally correct but also legally and ethically ready.
- Device and Compatibility Testing:
Telehealth apps run on many kinds of devices – different Android phones, iPhones, tablets, web browsers, etc. Do a compatibility matrix and test on a variety of devices:- Different screen sizes and OS versions (especially if you promised support for older versions, test on say Android 8.0, 9.0, etc., and iOS one version back from current).
- Different browsers (Chrome, Safari, Firefox, Edge) for the web app, and ensure things like video and audio work on each (especially Safari can have quirks with WebRTC, for example).
- Test the integration with peripherals if applicable: e.g., does the app work well with Bluetooth stethoscopes or otoscopes if those are used? Does it handle switching audio input from phone to bluetooth headset smoothly during a call?
- Also, since telehealth might involve connecting to a hospital’s systems, if you have any integration, test that thoroughly in a staging environment with real-like data. For instance, test pulling a sample patient record via FHIR – does it populate correctly in your app? Test sending a note back – does it arrive in the EHR?
Quality Assurance Process
Have a structured QA process in place. This includes having test plans and test cases for all features, maintaining a bug tracking system (JIRA, etc.) where issues are logged and resolved, and using test automation where practical. Automate repetitive tests like regression tests for APIs or even UI flows (with tools like Selenium or Appium) to quickly catch if a new change broke something that was previously working. However, manual testing is still very important, especially for UX and anything involving the human element (like actually seeing/hearing how a call performs).
Prior to a production release, consider doing a soft launch or a controlled rollout (like releasing the app to a small percentage of users or one clinic) to monitor for any issues, then scaling up.
Ensure QA also covers fail-safes: for example, if a video call fails, does the app provide info to the patient (“If you’re having trouble, call this number to speak to support”)? Or perhaps seamlessly switch to a phone call? Testing such fallbacks is part of a robust QA.
Essentially, telehealth testing must be rigorous and comprehensive. It's not just "Does the app meet the specifications?" but also "Does it meet users' needs in the field? Is it safe and reliable under all conditions?" As Arkenea notes, ensuring your app works flawlessly is a significant milestone in the development process. Allocate ample time in your project plan for quality assurance (QA); don’t cut it short to rush deployment. Any bugs in a live healthcare setting can quickly erode trust. Investing in a strong QA phase (and ongoing QA for updates) ensures high quality, which differentiates your app in a sensitive market like healthcare. A well-tested telehealth app gives patients and providers confidence that they can rely on virtual care without any problems.
Step 8: Deployment and Integration

With development and testing completed, the next stage is deploying your telehealth app to production and integrating it into the real-world healthcare environment. Deployment is not just about pushing code to a server or app stores – in healthcare, you need a reliable operations setup and a plan for how your app will integrate with users’ existing systems and workflows. Additionally, you must plan for ongoing support, maintenance, and scaling as your user base grows. Let’s break down the key considerations for deployment and integration:
Cloud Deployment & Hosting Setup
As discussed in Step 3, you likely will deploy on a HIPAA-compliant cloud infrastructure (AWS, Azure, GCP, etc.). Now is the time to finalize your production environment:
- Set up your production servers with proper configuration – use infrastructure-as-code scripts so that your production mirrors what you tested (but with production-scale resources). Enable all security configurations: e.g., enforce HTTPS only, install your SSL/TLS certificates, configure firewalls/security groups to only allow necessary traffic (open video ports if needed, etc.).
- Implement your CI/CD pipeline to production. Ideally, you have automated deployments – maybe code merged into the main branch goes through tests and then can be deployed with one click or automatically. Many teams do gradual deploys (like canary or blue-green deployments) to ensure stability.
- Ensure logging and monitoring are active on production. Use cloud monitoring to keep an eye on server health (CPU, memory), and application performance metrics (API response times, etc.). Set up alerts – e.g., if CPU usage goes above 80% for 5 minutes, an engineer gets notified, or if the number of errors in logs spikes, an alert triggers. Remember, you might have critical operations at stake (doctors in calls), so you want to catch issues ASAP.
- Also plan for data backups in production: configure automated backups for databases (with encryption). Test the backup restoration process as part of deployment readiness.
- For mobile apps, prepare for App Store and Google Play deployment. This means creating developer accounts (if not done), preparing store listings (description, screenshots), and going through the review processes. Apple’s App Store in particular will review your app; mention in the notes that your app is a telehealth platform and describe any special usage. Ensure you comply with their guidelines (e.g., if you use in-app payments vs. external payments – healthcare apps often are allowed to let users enter insurance/payment info externally).
- Deploy web app on a secure domain (like https://yourapp.com), and ensure compliance with regulations like having a privacy policy page, terms of use, etc., accessible from the app.
Integration with Healthcare Systems
Once in production, your app likely needs to connect with external systems in real usage. Integration can include:
- EHR Integration: If you’ve built connectors to Electronic Health Records (via FHIR or HL7), coordinate with the healthcare providers or hospitals using your app to integrate it. This might involve getting API credentials from an EHR vendor or doing a deployment of a small middleware in the hospital’s environment. Ensure that any integration is deployed securely (no open access to your endpoints without auth, etc.).
- Third-Party Services in Production: Activate production API keys for services like Twilio (for video or SMS), Stripe (for payments), etc. Many have separate test and live credentials – double check you’re using the live ones now and that they are properly configured (e.g., Twilio needs configuration for TURN servers possibly, Stripe needs webhooks set to production URL, etc.).
- Telecom/Network Integration: Some telehealth providers integrate with telecom systems (for dial-in phone bridging, etc.). If you have such features, coordinate with those providers to ensure numbers are provisioned and calls route correctly.
- If integrating medical devices, ensure the production systems (device cloud accounts or keys) are ready. For example, if connecting to a Fitbit or Apple Healthkit, go through their production app approval processes.
- Sometimes integration means customizing per client: e.g., one clinic might want your app to send data to their analytics system. These are often handled on a case-by-case basis. Design your system to be flexible (maybe via webhooks or APIs that you or the client can configure).
- Standards and Testing: If you use HL7/FHIR integration, consider going through certification if available (some countries have conformance tests). In the US, there's an ONC certification for health IT – depending on your product’s scope, you might pursue that in the integration phase to prove it plays nicely with others.
Continuous Deployment and Updates
Telehealth apps will need frequent updates (for new features, security patches, adapting to new regulations). Set up a continuous delivery process so that deploying updates is routine. For mobile, you might not push updates as often (since users have to download new versions), but plan perhaps a release every few weeks or as needed. For web, you can deploy much more frequently since it’s under your control.
- Use a staged rollout for mobile updates – e.g., release to 10% of users, monitor crash logs, then release to everyone. This way if a bug slipped through, it impacts fewer people.
- Always monitor your app after each deployment for any unusual errors or user complaints.
- Have a rollback plan – if a new release causes major issues, ensure you can revert to the previous stable version quickly.
Support and Maintenance
Once users are on-board, you need to provide customer support and technical support:
- Have a process for user inquiries or issues – perhaps an in-app support chat, a support email, or a ticket system. For medical apps, users might raise issues like “video quality was poor” or “prescription didn’t reach pharmacy”. Your support team should be trained to handle basic troubleshooting (check internet connection, ask if the user is on latest version, etc.) and escalate real technical issues to the engineering team.
- Offer training or onboarding for provider users if needed – sometimes a quick guide or webinar for clinic staff can smooth the integration of your app into their practice. You may deploy with some training materials or an FAQ knowledge base for common questions (“What do I do if a patient doesn’t join the call?” etc.).
- Keep server OS, libraries, and dependencies up-to-date (within a schedule that doesn’t disrupt service). Monitor usage to see if you need to increase server capacity. Over time, archive or purge data as per retention policies (maybe writing scripts for that).
- Keep an eye on regulatory updates: for instance, if cross-state license waivers expire, you may need to update your app to enforce that. Or if new telehealth billing codes come, update those in the system.
Scaling and Optimization
Hopefully, your telehealth app will grow in users. Plan for scaling:
- From a technical perspective, use the cloud’s auto-scaling features. For example, set up auto-scaling groups that can add more server instances if CPU or network load goes high. Ensure your architecture is stateless enough (or uses a shared session store) to allow load-balanced scaling.
- Database scaling: as data grows, you might need to move to read-replica databases or a cluster. Monitor performance and do capacity planning.
- Geographical scaling: If you start in one region and expand globally, deploy additional instances in new regions (e.g., an EU deployment to keep EU data local, an Asia-Pacific one for latency improvement). Cloud providers make it relatively easy to spin up in new regions, but you’ll need to manage data segregation and perhaps separate configurations.
- Cost optimization: Keep an eye on cloud costs as you scale – telehealth (with video especially) can rack up bandwidth and compute costs. Optimize where possible: e.g., automatically shut down video session when not in use, compress data efficiently, leverage cheaper storage tiers for old records, etc.
Real-World Integration
Integration is not just technical; it’s also process integration. Work closely with the healthcare organizations using your app to integrate it into their clinical workflow:
- For example, ensure that when a telehealth appointment is scheduled in your system, it also appears on the clinic’s schedule (via integration or at least an email notification) so they don’t double-book a doctor for an in-person visit at that time.
- Provide any needed reports or data exports for the clinic’s records. Some clinics might want a monthly CSV of all telehealth visits for internal auditing or for insurance claim reconciliation. Make those available (with proper security).
- If the telehealth app is supplementing in-person care, integrate data flow: e.g., after a telehealth visit, perhaps a note should be sent to the patient’s primary care provider. Decide how that happens (maybe via integration with their system or a simple secure email/fax).
- Communication channels: integrate with their patient communication – e.g., some clinics might want to send automated phone reminders too. If so, maybe integrate your scheduling with their robocall system or so. These are often custom per client.
Post-Deployment Monitoring and Improvement
Once deployed, it's not the end – you now gather real usage data and iterate:
- Monitor KPIs such as number of consultations completed, average call drop rate, average wait time in waiting room, etc. These metrics will show how well your platform is working. For instance, if you see many users start a call but drop off in 1 minute, investigate if there’s a technical issue causing disconnects.
- Also monitor clinical outcomes if possible (though that might be longer-term) – e.g., patient satisfaction ratings, or did telehealth help reduce ER visits for that client? These are more for the value proposition but can guide integration improvements.
- Solicit user feedback regularly: in-app surveys or periodic meetings with key client stakeholders to see if the platform needs adjustments or new integrations.
Although deployment and integration may seem less glamorous than other aspects of software development, in healthcare, they are essential. Smooth deployment means patients can start receiving care and clinicians can easily adopt the tool. Good integration means your telehealth app becomes part of the healthcare ecosystem instead of operating in isolation. Taking the time to do things right — with robust hosting, a careful rollout, and strong support — will lay the foundation for your telehealth service's success and reputation.
How Intersog Can Help
Intersog is an experienced healthcare software development company that delivers custom telemedicine solutions tailored to your needs. Our teams specialise in:
- AI‑powered healthcare – We develop machine‑learning models for symptom checking, predictive analytics and conversational agents while ensuring data privacy.
- Full‑cycle telehealth app development – From discovery and user‑experience design to mobile/web development, API integration and deployment, our engineers build HIPAA‑ and GDPR‑compliant platforms with scalable cloud architectures. We use proven frameworks such as React Native, Flutter, Node.js and .NET.
- Integration & interoperability – We integrate telehealth apps with existing EHR systems using FHIR/HL7 standards, and connect wearables, RPM devices and third‑party services.
- Regulatory compliance – Our solutions meet stringent security requirements. We implement encryption, secure authentication, audit trails and help with documentation for HIPAA and international regulations.
Partnering with Intersog allows you to focus on clinical innovation while entrusting development to experts. Whether you need a minimum viable product or an enterprise‑grade telehealth platform, we can help you bring safe, user‑friendly digital care to market.
Leave a Comment